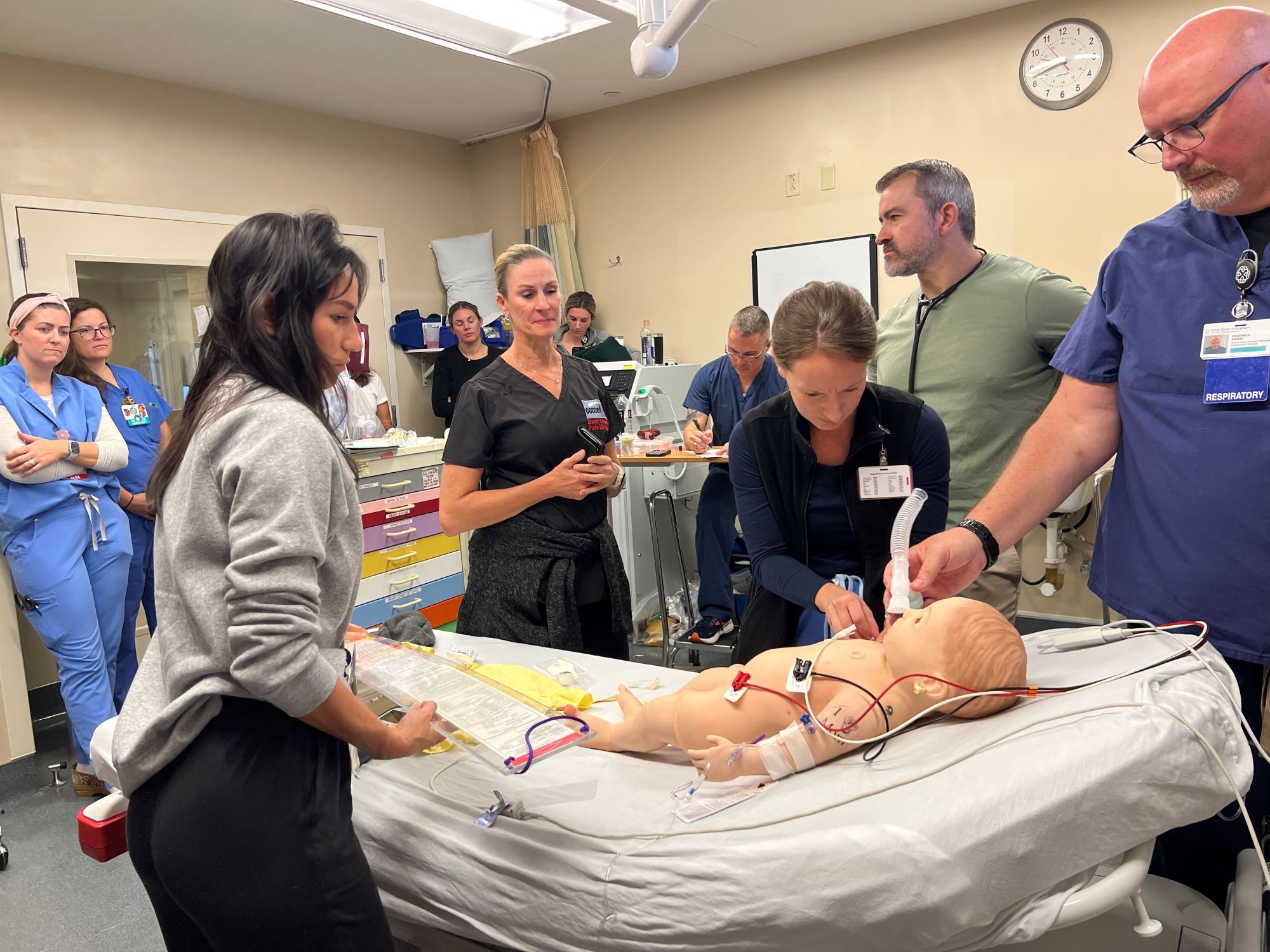
Dr. Jeffrey Zack, a Martha’s Vineyard Hospital emergency department doctor, and Dan Friedrich, Manager of Respiratory Therapy, huddled over an 18-month-old baby that was having difficulty breathing. The ambulance staff from Oak Bluffs had scant details on the precise health issues, but shared that the young Brazilian girl named Sadie is asthmatic.
In what might look like a chaotic scene to outside observers, nurses worked methodically to get vital signs and to prepare an IV while Dr. Zack gathered critical medical history from the mother.
When Dr. Zack mentioned the need to intubate, the mother’s concern grew.
“That sounds bad,” the mother said. “Do we really have to do that? Why?”
“She’s pretty sick. We want to make sure she’s going to be OK,” Dr. Zack responded.
The training scenario played out in a Martha’s Vineyard Hospital Emergency Room with more than a dozen nurses and ED staff observing and providing real-time feedback. Dr. Zack, Dan, and the nurses involved were working with a simulator made to look like an 18-month-old despite an “I love Mom” tattoo on the left arm. The pediatric emergency training was hosted at the Hospital and was led by Dr. Barbara Walsh, a Clinical Professor of Pediatrics at Boston Medical Center and part of the Community Outreach Mobile Education Training (COMET) program at BMC.
The COMET team works to provide healthcare professionals across Massachusetts with high-quality educational experiences focused around pediatric critical care. The training was held during Emergency Nurses Week, a time when the critical role played by these nurses in the health and well-being of patients is celebrated.
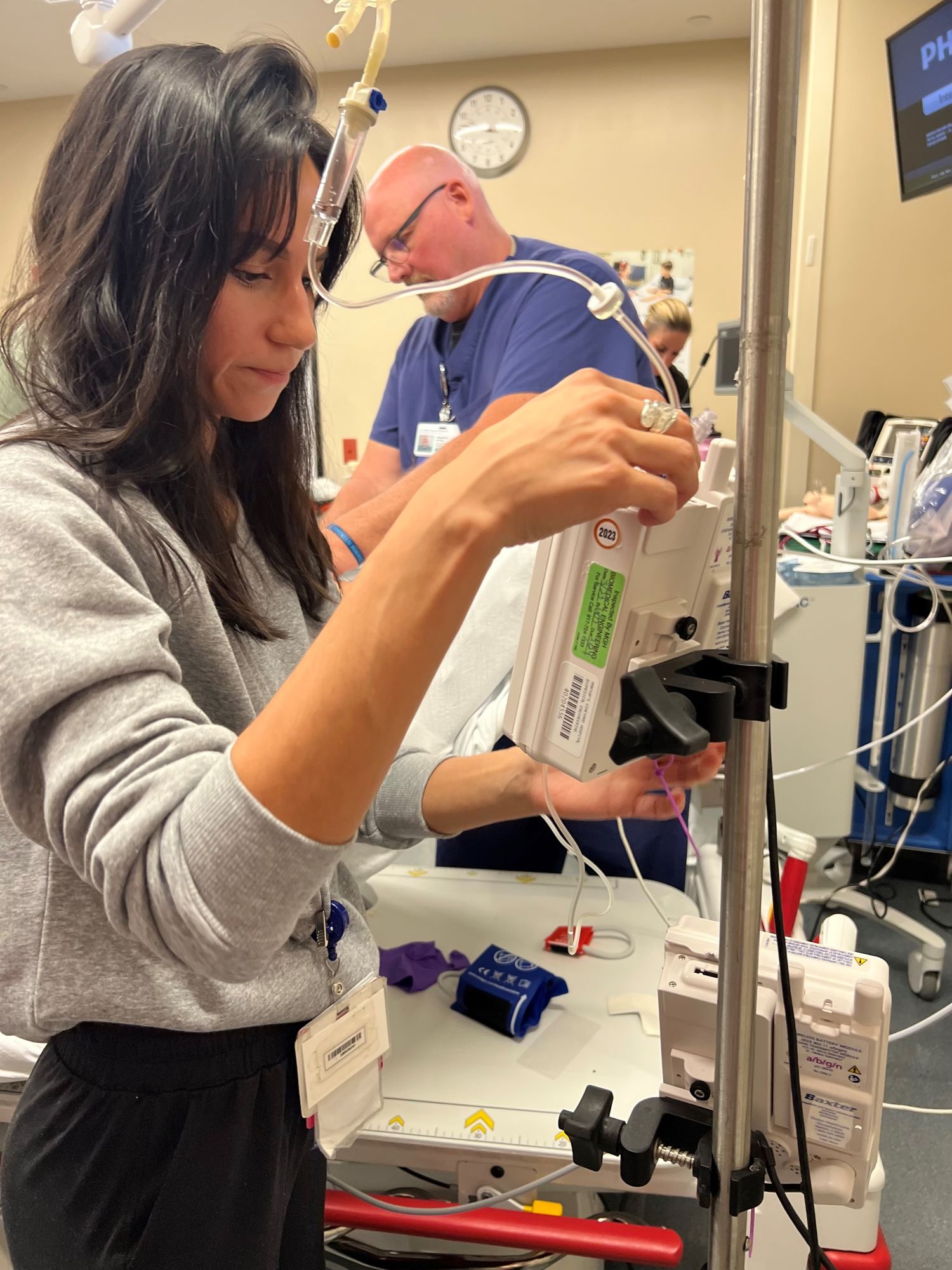
“This is crucial training for our staff who provide the highest level of pediatric care on the Island,” Ryn Gluckman, Nurse Director of the ED, said. “We try to provide this training to ED nurses at least once a year. This gives us practice not just with the all the aspects of clinical pediatric care, but also with our own communication and teamwork in high pressure events. This summer we had several very sick kids and the COMET training reinforces our skills and helps us to provide excellent and well-coordinated care to these children and their families.”
Gluckman added that the training is supported financially by the Massachusetts Department of Public Health because of MVH’s role as a critical access hospital.
Along with the case of the barely breathing baby, Dr. Walsh led the team through three other pediatric scenarios – all with one goal of preparing staff for the types of cases they might encounter on any given day in a chaotic ED setting. The other three scenarios included a precipitous delivery in the ED of a neonate, a toddler choking on a Lego, and a liquid nicotine overdose in a 6-year-old, Dr. Karen Casper, Emergency Department Medical Director, said.
Each session ended with a debriefing on what went right, what could be improved upon, and with some tips from observing emergency team members on what they might have attempted given the same scenario faced by Dr. Zack and his team.
“I like to do this case because respiratory season is upon us. These patients can be your worst nightmare,” Dr. Walsh explained. She kicked off a robust discussion by asking what biggest fear is with intubating an asthmatic child.
“Lung compliance,” one person said.
“Pneumothorax,” added another.
Dr. Walsh then asked if observers saw a change in the toddler during the scenario.
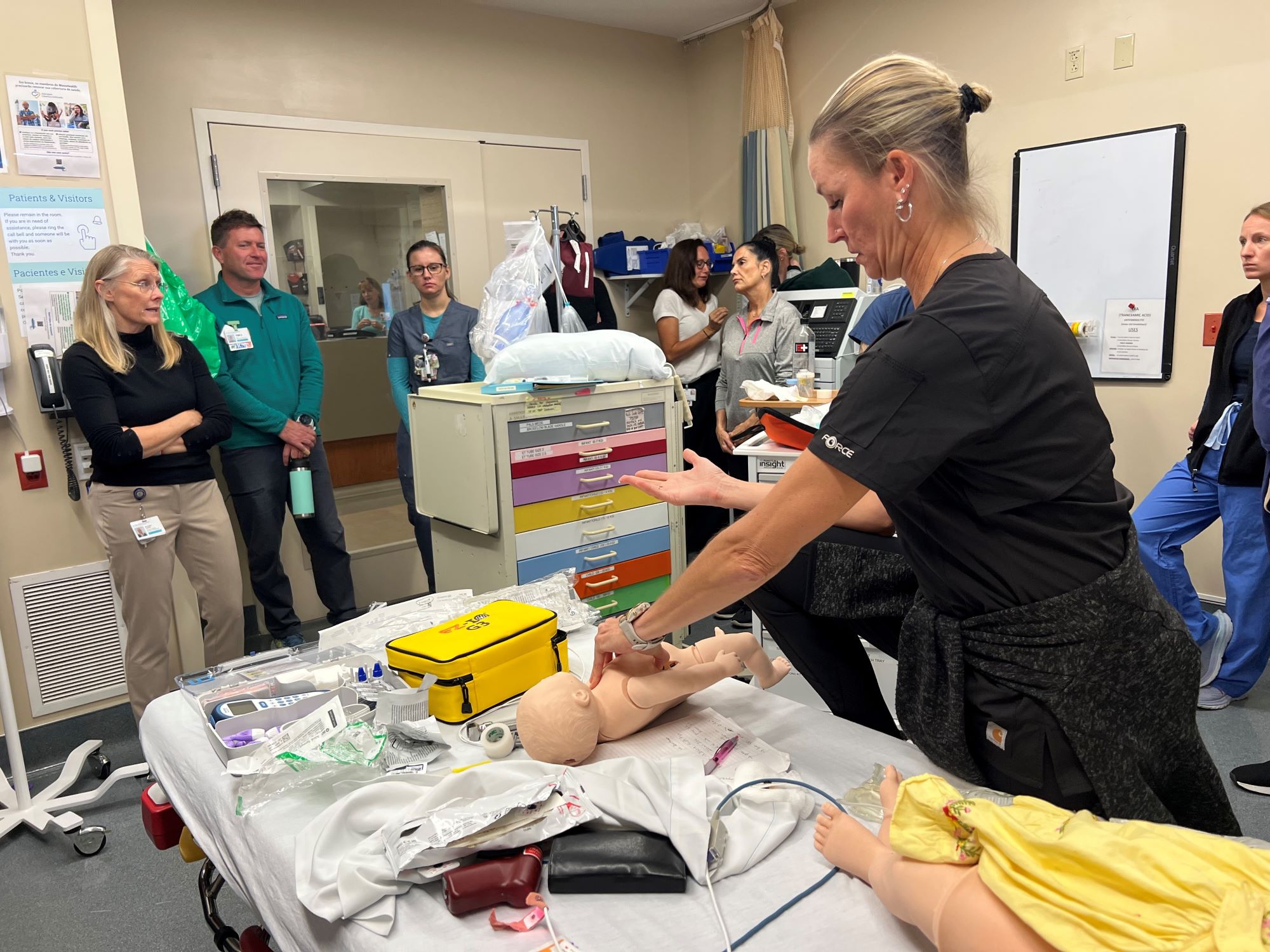
“Grunting,” said one.
“They’re auto-PEEPing. That grunt, that eh, they’re opening up their lungs by themselves because they’re really in failure,” Dr. Walsh said.
She also asked if any change in mental status was observed.
“The eyes started to close,” a nurse said.
“Yes!,” Dr. Walsh responded.
Dr. Walsh said children who are asthmatic present challenges because they’re already sick and that makes it difficult to get them back.
“If you prepare for the worst, it won’t happen,” she said. “When you don’t prepare for the worst, everything that could possibly go wrong will go wrong.”